Lecture by Mark Pettus transcribed by Carolann Patterson
INFLAMMATION: ARE YOU PLAYING WITH FIRE?
Learning Objectives from today's lecture:
- Explore the root causes of inflammation that fuel chronic-complex disease
- Examine the connection between inflammation and brain health
- Examine the mechanisms that link many common environmental triggers with increased inflammation
- Consider lifestyle changes that can reduce-reverse inflammation to improve longevity and quality of life
The proposition for this lecture: how the outside gets inside
- Health and disease are byproducts of complex individualized gene-environment interactions that may go back more than a generation before our conception and continue throughout our lives.
- Your DNA i.e., your “Book of Life” still has a Stone Age imperative, not often adapted for 21st century environmental inputs e.g. the foods in our modern food supply.
- This incompatibility creates a distorted metabolic trajectory e.g. inflammation that forms the basis of chronic complex disease and diminished quality of life.
- Through mindful living that aligns conscious choosing with what are are most designed to be in relationship with, our biology can be transformed to promote-restore optimal function and health throughout the life continuum.
Nutrigenomics studies the effects of food and food constituents on gene expression and focuses on the molecular-level interaction between nutrients and genome. It is where we look beyond “food as calories” and see food for what it is: information. Molecules of food have the power to influence life-sustaining pathways. Depending on the quality of a certain food, it will send information that will either trigger inflammation or reduce it.
Does the stress of our present diet create an epigenetic change in our health? Absolutely...
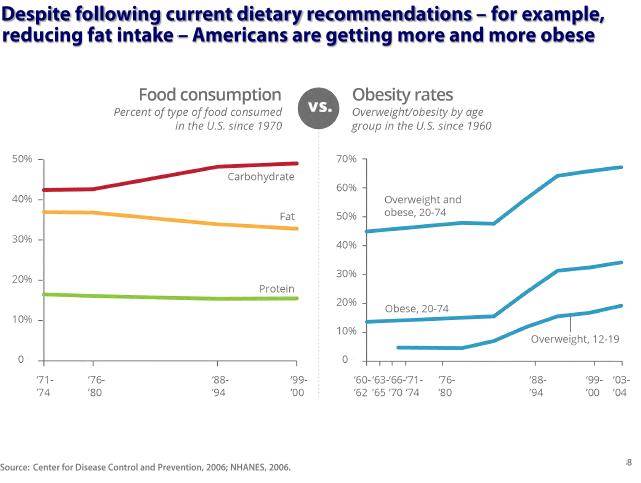
This is the shape of things to come…and this is the route we are taking to get there…
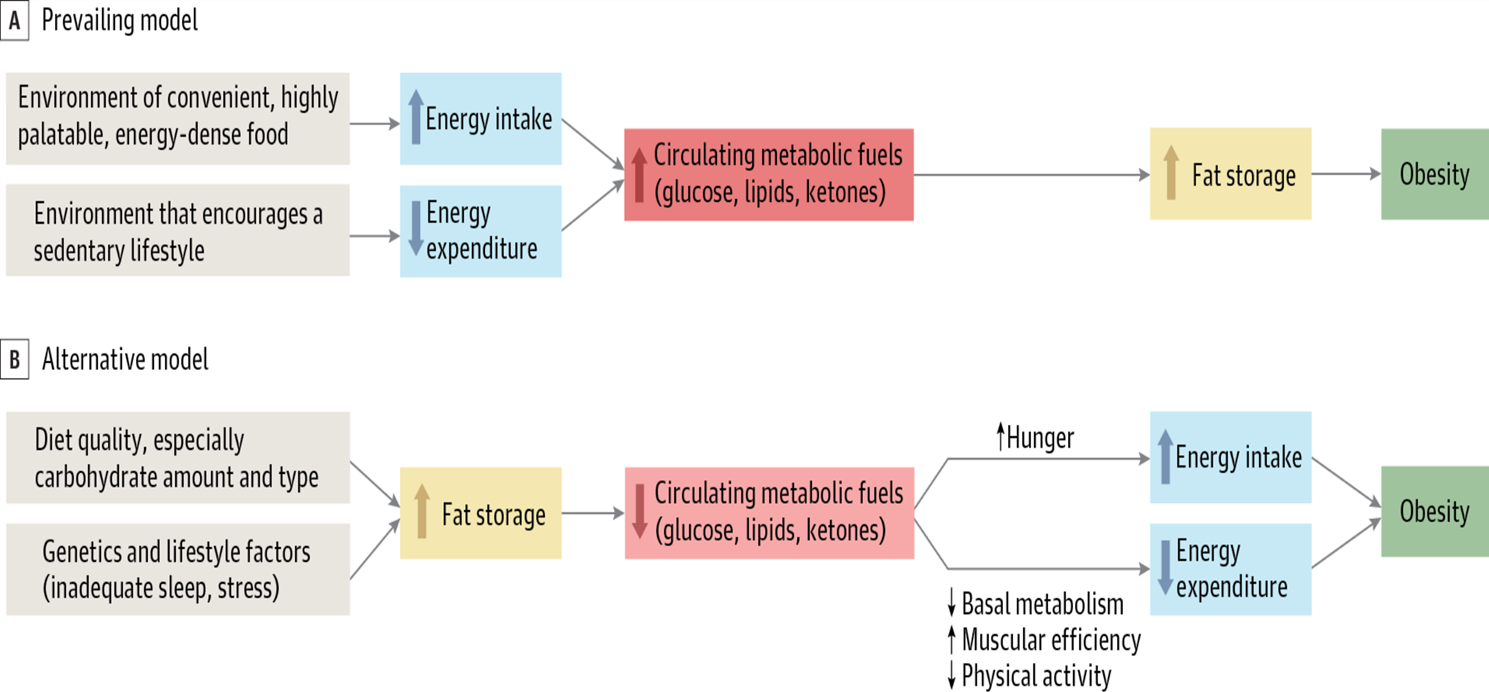
- Poor Quality Carbs - information from food leads to...
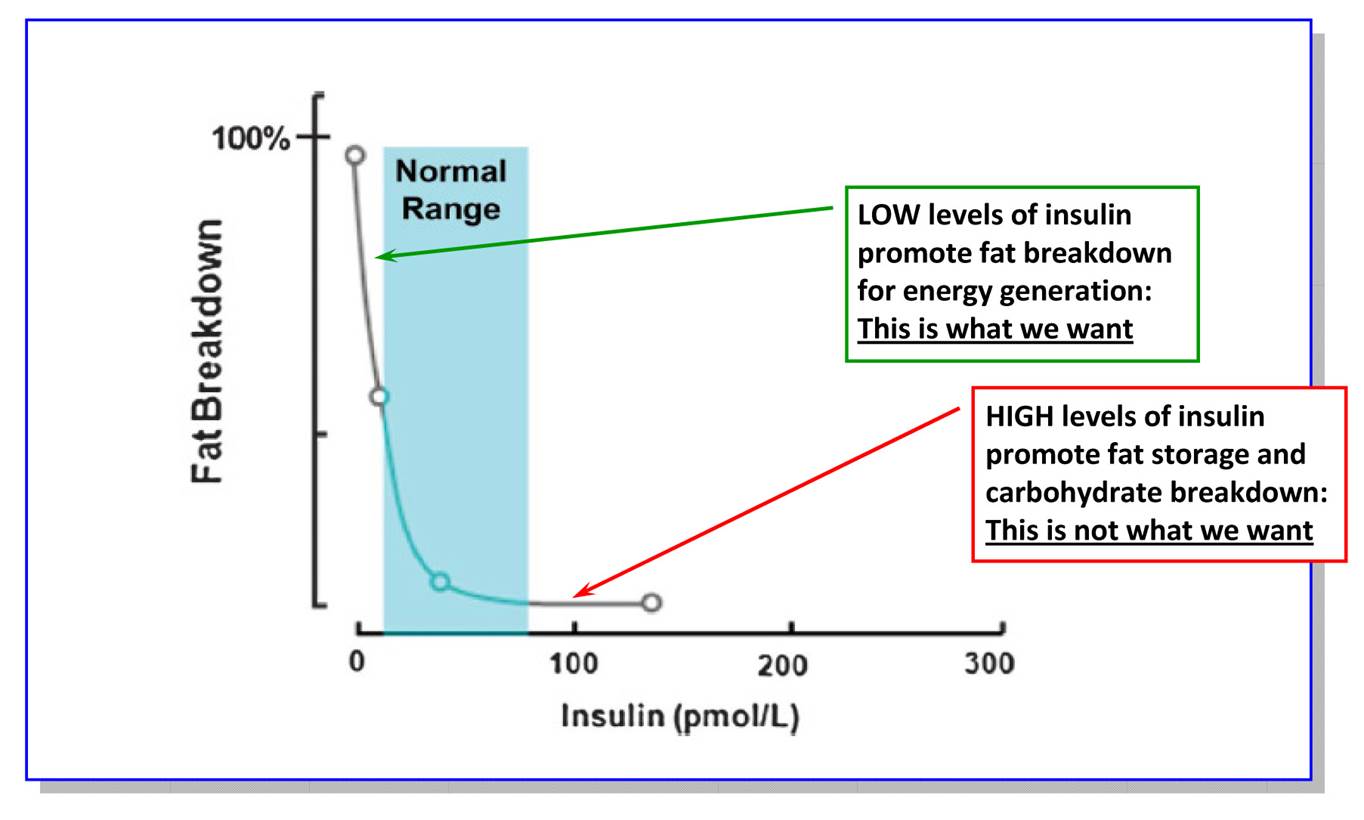
- Excess Insulin - It is impossible to burn fat with excess insulin [leads to...]
- Fat storage [leads to...]
- Down-regulation of insulin receptors [leads to...]
- Insulin Resistance and then on to Leptin Resistance and then on to Eat More + Do Less = NO GOOD
It is not simply a matter of poor food choices that lead to Inflammation and then on to Insulin Resistance. All of the following factors eventually lead to Insulin resistance: Visceral fat, Changes in food consumption, Stress, Sleep disruption, Altered gut-permeability/microbiome, Social Isolation, Hormonal imbalances, Toxin excess.
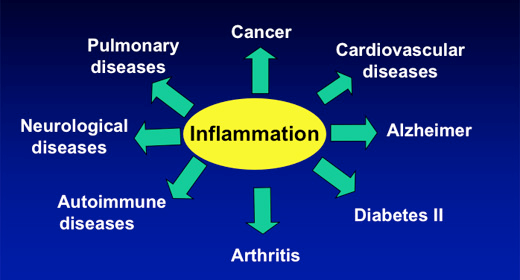
INFLAMMATION IS AT THE CENTER OF IT ALL
Inflammation is connected to every chronic complex disease...and it's got everyone's attention. Scroll through the titles listed below to find articles related to Inflammation and Stroke; Inflammation, Atherosclerosis and Coronary Artery Disease; Inflammation and Cancer; Inflammation and Depression and the Brain; Inflammation and Obesity; Obesity and Periodontitis.
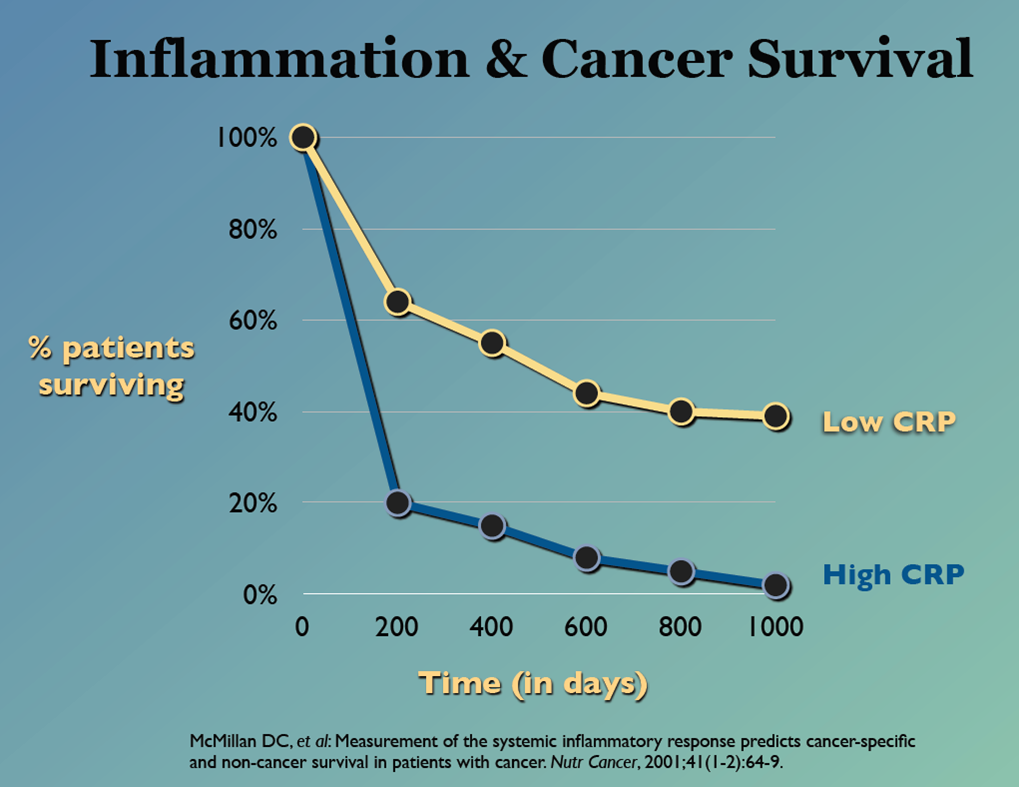
CRP. C-Reative Protein is a marker for inflammation. We can easily test for CRP levels. When tested for CRP, cancer patients' survival rates are higher when there is Low CRP. See graph below:
Slide courtesy Jeanne Wallace PhD
Inflammation effects cancer prognosis and reaction to chemotherapy: Patients with higher CRP experience poor prognosis; toxicity of chemotherapy; cachexia; and fatigue...
NF-κB is Inflammation’s “Master Switch” - keep it turned off
NF-κB is a nuclear transcription factor that is triggered by diet, stress, environmental toxins, visceral fat, infections, intestinal barrier integrity disruption, oxidized LDL, free radicals, vitamin D deficiency, altered microbiome, LPS, inflammation from other sources. It up-regulates expression of 400+ genes involved with cytokine production, cell proliferation, apoptosis, angiogenesis. Exercise, meditation, Vitamin D, Spices [e.g. turmeric] and many plant flavonoids have shown to inhibit NF-κB in vitro and in vivo.
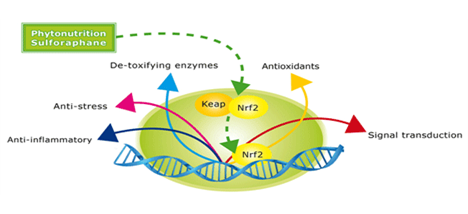
Nrf2 is the antidote to NF-κB.
Nrf2 activation is a critical intra-cellular defense: keep it turned on. Exercise, Meditation, EGCG, Resveratrol, Coffee, Sulfurophane, Curcumin all boost Nrf2.
FOOD AND INFLAMMATION
Changes in our diet trigger inflammation. Watch out for the following inflammation boosters:
- SUGAR and REFINED grain flours, PROCESSED poor quality carbs with high “carbohydrate density”FRUSCTOSE from sugar and High Fructose Corn Syrup
- Not enough vegetables and plant-based fiber to strengthen and balance your microbiome [we need 6-9 servings per day]
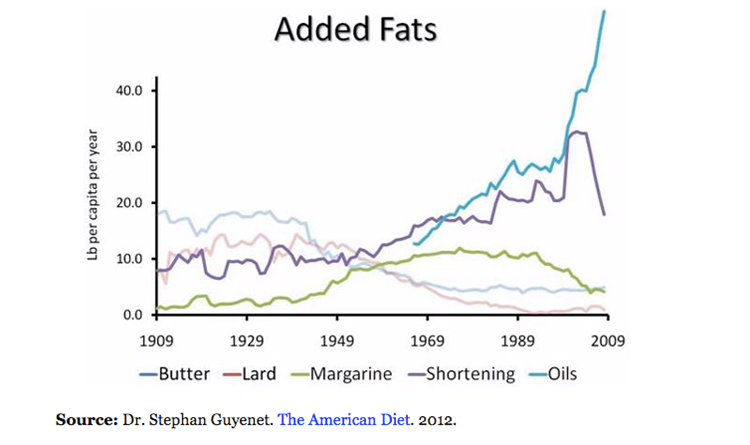
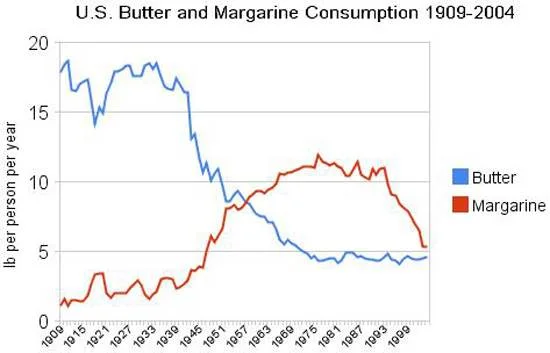
- Increased processed seed oils [they are too high in Omega-6 polyunsaturated fatty acids. Excess Omega-6 fatty acids build up in our cell membranes and contribute to inflammation]
- Insufficient healthy saturated fat [e.g. coconut oil and grass-fed-pasture-raised butter, whole milk, cream, eggs, red meat]
- Sensitivity to GLUTEN and DAIRY
- ENVIRONMENTAL TOXINS - contaminated foods such as game fish [mercury], non-organic fruits and vegetables [pesticide residues], food stored in BPA in plastics…and that’s just the short list
SUGAR
Obesity and Diabetes: The Twin Epidemics. Rates of Obesity and Diabetes have risen drastically in the past century. In 1890, one in thirty [adult 60 year old men] was obese. In 2000, 1 in 3 [adult 60 year old men] was obese. In the 1930's, one in 50,000 adults was diabetic. In 2000, one in 9 adults is diabetic [Johnson et al, American Journal Clinical Nutrition, 2007].
Inflamed About Obesity, Michael Lehrke & Mitchell A Lazar: Two studies find that adipocytes and macrophages have more in common than previously thought. The work bolsters the notion that the inflammatory response might link obesity to afflictions such as diabetes. The epidemic of obesity stems from a clash between genes that allowed our ancestors to survive extended periods of famine and the caloric excess and sedentary lifestyle of our modern environment. Obesity is a major risk factor for diabetes and atherosclerosis, afflictions associated with a constellation of insulin resistance, hypertension and lipid abnormalities that is now defined as Metabolic Syndrome [Nature Medicine, Vol 10, No. 2, February 2004]
What is metabolic syndrome? Metabolic syndrome is not a disease in itself. Instead, it's a group of risk factors- high blood pressure, high blood sugar, unhealthy cholesterol levels, and abdominal fat at the following levels [Source AHA]:
- Waist Circumference > 35” in women and > 40” in men
- BMI > 30 (= obese)
- Elevated blood pressure: > 130/85
- High triglycerides: > 150 mg/dL
- low HDL: < 40 mg/dL men, < 50 wome
- Elevated fasting glucose: >100 mg/dL
Visceral Adipose stores [mid-section weight gain, belly fat] is linked to Insulin Resistance; Dyslipidemia [high TGA and low HDL]; Elevations of Blood Pressure; and increased risk of chronic complex disease. It is the outward signal that internal fat surrounds organs and can penetrate the liver, causing the liver to respond as though it is Hepatitis.
The Quality of carbohydrates you eat matters.
Different carbohydrates produce unique genomic responses. NF-κB is the Inflammation Master Switch: keep it turned off...
High Glycemic Carbs [NF-κB turned on = bad].
Low Glycemic Carbs [NF-κB turned off = good].
... and stay away from those seemingly innocent rice cakes and pretzels!
GLUTEN
Gluten attacks the intestinal tract. Boston Mass General's Alessio Fasano is a gastroenterologist and pioneering researcher whose team discovered Zonulin, the molecule which regulates intestinal permeability, a.k.a. Leaky Gut.
Gluten triggers Zonulin. Over-production of Zonulin has been linked to a series of autoimmune diseases, including Type 1 Diabetes, Celiac Disease and Multiple Sclerosis.
Gluten is the primary cause of Celiac Disease. Fasano's research in 2003 demonstrated the prevalence of Celiac Disease in the U.S. to be far higher than previously thought, at a rate of 1 in 133 persons. Currently, 1.4% of Americans have Celiac Disease.
Primary source of Gluten is Wheat, and Wheat is NOT what it used to be...
GLUTEN MIND and GLUTEN MOOD
Inflammation is a systemic process. Inflammatory triggers such as Gluten cause inflammatory manifestations in all parts of the body, not just at the "point of entry" e.g. the stomach and can disrupt coordination/balance, cause joint pain and brain fog and...
- Celiac Disease is caused by Gluten and associated with many neuro-psychiatric diagnoses e.g. ADHD seen in approx. 60%!
- Celiac Disease is associated with white matter changes on MRI…similar to that seen with MS
- Gluten increases insulin resistance in individuals who are sensitive
- Brain wave patterns in ADHD improve consistently with gluten restriction
- Gluten sensitivity enhances zonulin that increases intestinal permeability
- Gluten sensitivity can alter blood flow to frontal lobes
From Gut to Brain: Gluten sensitivity is linked to:
- Dementia
- Depression
- Headaches
- Movement disorders
- ADHD
- Pain
The intestines are only one cell layer thick. What causes Intestinal Permeability?
- Food sensitivities
- Dysbiosis – Too much bad and not enough good bacteria. Gut microbiome needs diversity to balance
- Acid suppression [Causes overgrowth of bad bacteria. Prolonged acid suppression is not good for you Short-term use only e.g Prilosec]
- Stress response
- Environmental toxins
- Medications e.g. regular steroids and NSAID use [irony: anti-inflammatory drugs such as Tylenol and Ibuprofen promote inflammation]
A-cellular carbohydrates [not from vegetables or legumes] cause increased inflammation which leads to:
- Insulin-fueling lipogenesis
- Insulin resistance in muscle and liver
- Inhibits capacity to burn fat
- NF-κB goes up [bad]
- Increased LPS - Lipopolysaccharides elicit a variety of inflammatory responses and may be a part of the pathology of Gram-negative bacterial infections [bad]
- Cytokine up-regulation [bad]
- Leptin resistance [hungry and less energy to move]
- Poor health and many symptoms [including Periodontal disease]
The Host Genotype Affects the Bacterial Community in the Human Gastrointestinal Tract
Host genes shape the gut microbiota. 90% of our bodies is not human: it's microbial. Microbes are essential to our health and most of them live in the gut sending out messages to support digestion, immunity, metabolism. When the microbiome is disrupted and out of balance [dysbiosis] messaging in our body gets mixed up. Big time.
The F-Word: FIBER [and F. prausnitzii]
When the mucous layer in the intestines is reduced, opportunists can move close to the gut lining, inciting inflammation. Fermentation of plant-based fiber seems to keep the mucous layer intact. So does the presence of peace-keeping microbes such F. prausnitzii.
Speculative interpretation of current research is that gut colonization is most beneficial before the age of 3 and is strengthened by these three key factors at birth to age 3:
- Vaginal delivery
- Breast-feeding
- Minimal or no use of antibiotics and anti-bacterial products [both contribute to a less diverse ecosystem and microbiome]
Diversity of gut colonization relies on:
- One organism preventing overgrowth of another
- Cross-talk influencing the immune system
Late colonization/infection + poor microbial diversity + genetics = sickness
Scientific America explains why our progeny may not be inheriting their fair share... "Because the critical issue is the inter-generational transfer of microbes and its timed assembly, three periods are relevant: before pregnancy, during pregnancy and in the child's early life.
For all three periods, antibiotic use is relevant because it may directly change maternal microbes prior to transfer or the child’s microbes afterward. Elective cesarean sections mean that the child misses the birth canal transit, and anti-bacterials in soaps and foods directly affect microbiota composition. Infant formulas have not been constructed with the benefit of millions of years of mammalian evolution, because breast milk contains nutrients that specifically select for the growth of preferred co-evolved organisms and inhibit opportunists and pathogens.
The aggregate of modern assaults on the early-life microbiome suggests that our progeny may not be inheriting their fair share. Exceeding the developing microbiome’s plasticity predictably leads to consequences, as growing evidence evinces.
Studies have linked C-sections and exposures to prenatal and postnatal antibiotics to increased risk of obesity, diabetes, celiac disease, asthma and allergies, among other ailments that have their roots in development."
PSYCHOBIOTICS
The brain responds to the gut. Researchers have learned which strains of gut bacteria affect the nervous system and have mapped out the pathways they use to influence the brain. Gut flora can improve mood; some can produce neurotransmitters such as norepinephrine, serotonin, and dopamine; while other microbes such as L. helveticus and B. longum operate through the neuro-endocrine system and can lower cortisol.
A specific strain of Lactobacillus reuteri can increase the level of oxytocin, the hormone that kicks in when you cuddle, hug, or have sex. Lactobacillis acidophilus [found in yougurt, sauerkraut, and kimchi] is critical to regulating pain. B infantis and L reuteri and other strains attack inflammation by suppressing pro-inflammatory cytokines. They also send signals to increase Leptin [The “I am Full” hormone].
Watch this space – Psychobiotics might just be the next happy pill because of their links to:
- Protection of intestinal barrier function
- Influence on local and systemic antioxidant status
- Direct neurochemical production e.g. Gamma Amino Butyric Acid
- Indirect influence on neurotransmitter function
- Experimental evidence of links to depression, anxiety, and autism
- Stress-induced alterations in microbiota
- Direct activation of neural pathways between gut and brain
- Regulation of immune response - inflammatory cytokines
- Can influence production of Brain Derived Neurotrophic Factor [BDNF]*
- Loss of microbiome “heritage” a contributor to many modern diseases
[Psychobiotics: a novel class of psychotropic. Biol Psychiatry. 2013 Nov 15;74(10):720-6. doi: 10.1016/j.biopsych.2013.05.001. Epub 2013 Jun10. Fermented foods, microbiota, and mental health: ancient practice meets nutritional psychiatry Eva M Selhub1*†, Alan C Logan2† and Alison C Bested3 Journal of Physiological Anthropology 2014, 33:2]
*BDNF - Brain Derived Neurotrophic Factor
Up your Game and Up your Brain. Your Brain Derived Neurotrophic Factor [BDNF] is Known as "Miracle Grow." BDNF is decreased in Depression, Alzheimer's, Epilepsy, Schizophrenia and OCD.
BDNF increases with Exercise, Coffee [and other phytonutrients], DHA-omega 3, Curcumin-turmeric, EGCG [green tea], Meditation, Reduction in gut permeability.
Evidence for increased inflammation in:
- MCI/Alzheimer’s disease
- Depression
- Pain
- PD
- MS
- ADD and ADDHD
- Brain fog i.e., trouble with concentration, focus, memory
- Anxiety and Panic
- Autism spectrum
What is happening in the brain doesn't necessarily originate there.
The contemporary convergence:
Gene-Epigenome + Environment + Microbiome =
OUTCOME [how the outside gets inside]
Sugar triggers inflammation. Diabetes and pre-diabetes prevention and glucose control in midlife may protect against late-life cognitive decline. Higher glucose levels are associated with an increased risk of dementia. Studies show higher levels of fasting plasma glucose correspond to a higher rate of shrinkage of memory center [Neurology 2012;79:1019-1026].
High glucose is reversible and highly preventable.
High intake of energy from carbohydrates and low intake from fat may have inverse implications for development of Mild Cognitive Impairment [MCI]. In a study of 1,230 individuals age 70 and older, individuals with higher carbohydrate intake had nearly four times the risk of developing Mild Cognitive Impairment. Those individuals with the highest fat intake compared to the lowest fat intake were 42% less likely to have MCI.
MOTION is the LOTION:
Exercise training increases the size of the hippocampus and improves memory. "A physical activity program of an additional 142 minutes of exercise per week on average modestly improved congnition relative to controls in older adults with subjective and objective memory impairment" JAMA, September 3, 2008, Vol 300, No 9.
A six-month exercise intervention influences the genome-wide DNA methylation pattern in human adipose tissue. Studied followed 24 healthy men with low level baseline activity levels before and after 6-month exercise program. There were 30 controls as genome-wide methylation patterns were examined in adipose tissue. Several patterns changed in exercise group demonstrating reduced lipogenesis and a “silencing” of genes associated with obesity, inflammation and impaired insulin signaling.
SLEEP WELL
Disrupted sleep and loss of entrainment is a major inflammatory risk
- 15% of Americans experience insomnia
- 1 out of 3 has sleep disruption on one or more nights each week
- Major risk factor for many chronic complex diseases
- Neuro-endocrine-immune disruption
- Sleep hygiene
- Obstructive Sleep Apnea
- Avoid pitfalls of sleeping medications
- Follow the Circadian Rhythm strategy [below] and work up to a healthy sleeping pattern:
ALLOSTASIS
The process of achieving stability or balance through physiological or behavioral change in response to changes in one’s environment. Simply put: Ability to achieve stability through change. Here are some helpful tips that are at the heart of an an Anti-Inflammatory Lifestyle:
- Sleep well. Get your ZZZ's and your Zeitgebers [Time Givers] - Light, Ambient temperature, Social Interactions, Exercise, Meal Timing
- Get your Vitamin D through supplements or sensible sun exposure each day. Vitamin D influences many things - Cardiovascular Disease, Cancer, Autoimmunity, Depression, CHF, Osteoporosis, Fall Risk, Pain Syndromes
- Whole foods always trump processed foods
- Reduce-eliminate sugar, fructose and refined-processed, grain-based flour [carbohydrate-dense foods] e.g. breads, pasta, bagels, chips, pretzels, muffins, donuts, and many cereal grains
- Consider an elimination trial e.g. gluten, dairy, sugar
- Eat lots of vegetables, plant-fiber, sweet potatoes, plantains, beans
- Reduce processed seed-vegetable oils e.g. corn, safflower, sunflower, canola, peanut and introduce more healthy fats e.g. grass-fed butter, EVOO, coconut oil, lard, ghee, and an increase in O-3s fatty fish, nuts, seeds, avocados
- Lean, red meat (grass fed-finished ideal), eggs
- Eat organic for “the dirty dozen” produce
Round off an anti-inflammatory lifestyle with these healthy practices...
- Movement: Motion is the Lotion: walking, aerobic, resistance, yoga, tai chi
- Mind-Body awareness
- Prayer, Breathing techniques, Relaxation Response, Meditation
- Mindfulness-based stress reduction; HRV-Heartmath
- Sleep hygiene-entrainment
- Laughter
- Volunteer Work
- Social connection
- Cultivate meaning in work, love, and play
- More time outdoors during sun season
Recommended Reading:
The Wahls Protocol, by Terry Wahl, M.D.
For more "news to use" and the science to go with it, visit The Health Edge: Translating the Science of Self-Care. Not all research slides are shown in this article. To download complete lecture, follow this link to BHS Creating Health Wellness Series.