Lecture by Mark Pettus transcribed by Carolann Patterson
Gastrointestinal Balance: Do you have THE GUTS for Health?
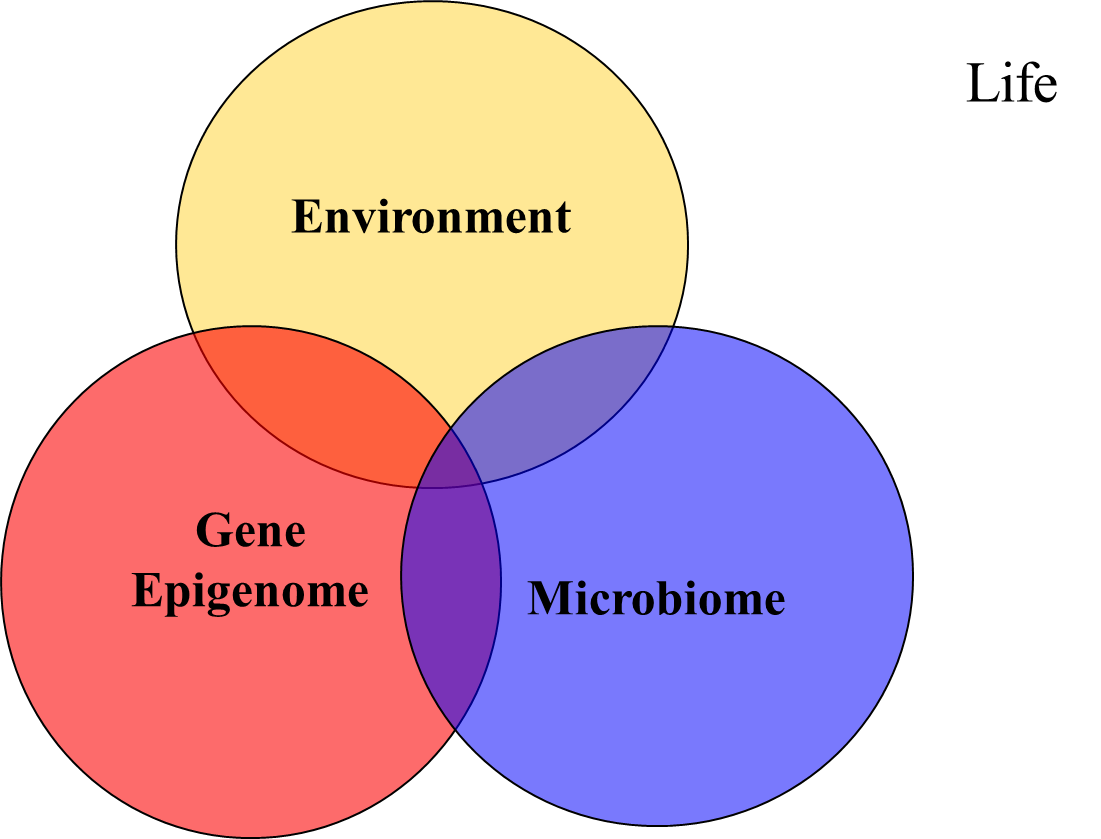
LIFE is comprised of tightly integrated relationships between our Environment [what do we eat, how do we move, what toxins are in our life, how much sleep do we get, how do we resolve conflict and manage stress?]; Gene Epigenome [our unique "Book of Life" which sets our body's on and off switches]; and our Microbiome [90% of our body is microbial]. We are not locked in to our genes and patterns - everything is modifiable.
Healthy choices in our Environment lead to healthy changes to our gene Epigenome and greater balance in our Microbiome. Everything is connected and overlapping. This approach is central to a Functional approach to your good health.
How does a Functional-Systems Biology Model differ from the way we are currently looking at our health? Instead of looking at "the leaves" of disease to determine treatment, Functional Biology turns the model on its head and shifts analysis to begin at the roots, to find the root causes. Once we discover the root causes we can change our biology by changing our behavior. Our DNA is more malleable than we think. We are NOT locked in to our genetic legacy.
Disease [how things appear] - Pre-Diabetes, Diabetes, Obesity, Metabolic Syndrome, Heart Disease, Stroke, Depression, Autoimmunity, Alzheimer’s, Cancer, Autism, ADD, Hypertension.
Core Metabolic Imbalances [what drives them] - Inflammation-Immunomodulation, Fight-Flight (HPA axis), Microbiome (Gut-Immune), Detoxification, Hormonal, Insulin resistance
Root Causes [what are their origins] - Gene-Epigenome Environment, Nutrition, Movement Stress Response, Environmental-toxins, Conflict Management Sleep, Social Connection, Traumatic events, Mindfulness, Meaning in Work, Love & Play
We don't get sick overnight. Disease is the accumulation of unhealthy choices, life patterns and events, and exposure to toxins over time. When we determine the root causes of Long Latency Disease [found in the roots], we can prevent disease from happening or make it disappear.
Our intestines are so much more than just a tube for digestion and absorption. The gut contents are an inner world that is “outside” the cellular body. Its surface is a frontier of 100 square meters and is only one cell layer thick. Your gut flora are an organ [the microbiome] that contains 10 times more microbial cells than the body has mammalian cells. Our microbiome has 100x the DNA than all of human DNA combined. From a cellular perspective, we are 10% human and 90% microbial.
Our gut is one cell layer thick. Most of our immune system is attached to the gut on the outside. It is poised and ready to attack threats.
The most sophisticated immunologic component in our body resides in the gut. A profound neuroendocrine connection exists within the Gut which is considered to be "the second brain" where 90% of serotonin in your body is produced. Our gut is one cell layer thick. Most of our immune system is attached to the gut on the outside, poised and ready to attack threats.
Digestive Disease impacts MILLIONS of Americans:
- 60-70% Americans suffer from Digestive Disease
- GERD effects 45-60 million
- 7-10% Americans experience heartburn at least daily
- 20% [60 million] experience at least once-monthly
- Irritable bowel disease [IBS] effects 30-45 million
- Gallstone disease, 20-25 million
- Diverticular disease, 20-40 million
- Celiac is estimated at 3 million, approximately 1:100 [up from 1:133 from 2003 Alessio Fasano study]
- Gluten sensitivity is seen in as much as 5-8% of Americans
- Crohn's Disease, 750,000-1 million
- Colerectal Cancer is approximately 260,000
Is your gut trying to tell you something? Yes.
100 million people experience various GI problems e.g. IBS, bloating, gas, reflux, constipation, diarrhea, and crampy pain. Americans spend $3 billion/year on OTC antacids, laxatives, acid blockers and fiber supplements [and some of the most popular prescription drugs used to alleviate digestive symptoms only exacerbate the cause, more on that below]. It is a common reason to seek medical care and a frequent reason for diagnostic testing...so yes, your gut is definitely trying to tell you something. The question is: WHAT is it telling you?
Problems with your gut health can promote and worsen the following conditions:
- Allergy
- Asthma
- Autoimmunity
- Arthritis
- Metabolic Bone disease
- Skin problems
- Mood disorders
- Dementia
- Cancer
- Inflammation
The Microbiome…it's an evolving story
The microbiome has evolved with humans. These "bugs" have allowed us to survive. The microbiome provides important functions in digestion, immunity, metabolism and detoxification. From a cellular perspective, our body is 10% human and 90% microbial. The gut microbiome in each person contains 100-150 times as many genes as the human gene pool and over 99% of the genetic diversity in our bodies is due to microbial colonization. 70% of the immune system is located in the gut epithelium [outer layer].
Gut microbes can drive appetite. Low Microbial Diversity in the gut drives obesity. Studies show that colonizing germ-free mice with the intestinal microbiome from obese mice led to an increased total body fat despite lack of change to diet.
Dirt is Good for Diversity. Increased diversity within the microbiome is seen with decreased hygiene. Early and diverse exposure to germs is key to a “healthy microbiome.” Reduced microbiome diversity is seen in obesity, IBD, and autism spectrum.
Diet is a powerful factor that can shift the gut microbiome. There is an increased carbohydrate digesting microbiome in populations with higher carbohydrate [CHO] intake.
SIBO - Small Intestinal Bacterial Overgrowth
SIBO is the root cause of many GI and systemic problems and is typically associated with carbohydrate intolerance and bloating after eating. It is also associated with:
Nausea, diarrhea, constipation
- Contributes to food allergies
- Intestinal permeability-systemic inflammation
- Present in 75% of people with IBS, fibromyalgia, CFS [Chronic Fatigue Syndrome]
- Eradicating SIBO often resolves symptoms of IBS
- Breath test is available
IBS - Irritable Bowel Syndrome
IBS is the most common GI functional disorder diagnosed by gastroenterologists and affects about 5-10% of the population with female predominance of 2-3:1. Its symptoms include abdominal pain, altered bowel function, bloating, mucosal inflammation, exaggerated stress response, increases in plasma pro-inflammatory cytokines. Stress [including early life stress] plays a major role in the onset and exacerbation of symptoms in IBS. It is closely linked to Dysbiosis [alterations, loss of diversity in microbiome], food sensitivities and SIBO [as many as 75%]. It is associated with:
- GERD
- Interstitial cystitis [inflammation of the bladder]
- Fibromyalgia
- Chronic Fatigue Syndrome
- Disrupted sleep
- Rosacea
- Migraine headaches
- Restless leg syndrome [RLS]
GERD [Reflux] - do we have it all wrong?
GERD has been thought to stem from too much acid and our approach has been to block acid production [a case of treating the "leaves" not the "root cause"], but with Reflux, there already is LOW stomach acid. Many who have GERD also have SIBO. The diagram below outlines how it works: Low stomach acid leads to bacterial overgrowth + maldigested carbs [from poor quality simple sugars] which create increased gas and pressure, pushing up towards the esophagus while also increasing IAP [Intra-Abdominal Pressure]. As SIBO breaks down the simple sugars [FODMAPS] it produces the gas that increases IAP that allows stomach acid to reflux into the esophagus.
Reflux is not a result of excess stomach acid. It is driven by LOW stomach acid. Prolonged use of PPI's - Proton Pump Inhibitors, such as Prilosec and Nexium - to alleviate symptoms of Reflux increases low levels of acid needed to properly digest food.
LPS - Lipopolysaccharide
Bacteria produce an endotoxin called lipopolysaccharide [LPS] from shedding their cell walls and induce inflammation. Researchers have found that gut-derived bacterial LPS enters the bloodstream and triggers insulin resistance that typically accompanies type II diabetes. Chronic high-fat [from bad fat] raises LPS levels and sets the stage for metabolic disease. LPS induces Leptin Resistance [the hormone that tells us we’re full].
Intestinal Permeability - Uncontrolled Trafficking of Molecules. How does the barrier break down?
- Dietary choices [reference Ian Spreadbury]
- SIBO
- Food allergies, lectins
- Dysbiosis [alteration in the gut, ANTIBIOTICS are the biggest contributor]
- ACID SUPPRESSION [PPI's not wise for long-term. We need acid to protect us and break down food]
- STRESS response [causes alterations in the gut]
- Environmental toxins
- Medications
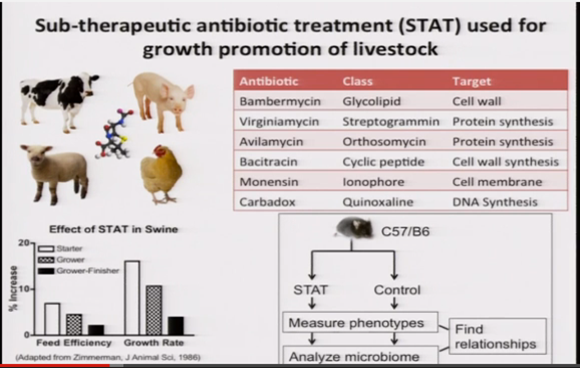
...Antibiotics on top of antibiotics - STAT food is neither ethical, nor healthy:
DIET - no lecture is complete without reference to Ian Spreadbury's research:
Ian Spreadbury points to the single greatest difference between ancestral and modern life: acellular carbohydrates. Wheat just ain't what it used to be.
WHEAT can be viewed as a Triple Threat from:
- Amylopectin - A high glycemic carb, a simple sugar that propagates an overgrowth of bacteria and yeast
- Gluten [for some]/gluteomorphins are an opiate-like substance
- Fructans - FODMAPs - simple sugars
Ingesting acellular carbohydrates [not from vegetables or legumes] increases inflammation and leads to:
- Insulin-fueling lipogenesis
- Insulin resistance in muscle and liver
- Inhibited capacity to burn fat
- NF-κB goes up [bad]
- Increased LPS - Lipopolysaccharides elicit a variety of inflammatory responses and may be a part of the pathology of Gram-negative bacterial infections [bad]
- Cytokine up-regulation [bad]
- Leptin resistance [hungry and less energy to move]
- Poor health and many symptoms [including Periodontal disease]
STRESS and the GUT
The Vagus Nerve is the largest nerve. It's a super-highway, central to all our systems and travelling in both directions between the brain and the gut.
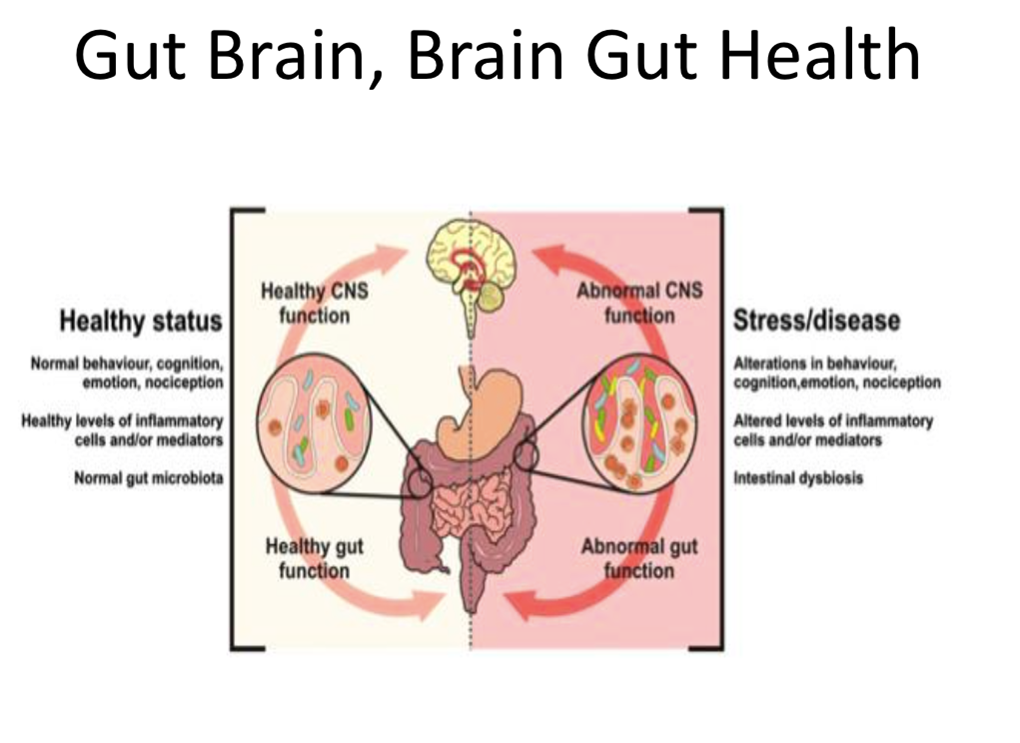
HEALTHY GUT and HEALTHY BRAIN = BALANCE
Mindfulness and balance are associated with healthy gut microbiome.
Depression, auto-immune, fibromyalgia [etc] are associated with STRESS, an UNhealthy gut and intestinal dysbiosis.
Host genes shape the gut microbiota. 90% of our bodies is not human: it's microbial. Microbes are essential to our health and most of them live in the gut sending out messages to support digestion, immunity, metabolism. When the microbiome is disrupted and out of balance [dysbiosis] messaging to the brain and throughout our body gets mixed up. Big time.
LEAKY GUT and GLUTEN
Gluten attacks the intestinal tract. Boston Mass General's Alessio Fasano is a gastroenterologist and pioneering researcher whose team discovered Zonulin, the molecule which regulates intestinal permeability, a.k.a. Leaky Gut.
Gluten triggers Zonulin. Over-production of Zonulin has been linked to a series of autoimmune diseases, including Type 1 Diabetes, Celiac Disease and Multiple Sclerosis.
Fasano's research in 2003 demonstrated the prevalence of Celiac Disease in the U.S. to be far higher than previously thought, at a rate of 1 in 133 persons. Currently, 1:100 Americans have Celiac Disease.
Gluten causes Celiac Disease and from this we know that Environment can impact our immune system. It may not just be gluten but other molecules, too, that play a role in digestive disease. WHEAT can be viewed as a Triple Threat from its contents - Amylopectin [a high glycemic carb, simple sugar that propagates an overgrowth of bacteria and yeast]; Gluten [gluteomorphins are an opiate-like substance]; and Fructans [FODMAPs - simple sugars].
GLUTEN aggrovates the gut and causes Inflammation
When the mucous layer in the intestines is reduced, opportunists can move close to the gut lining, inciting inflammation. Fermentation of plant-based fiber seems to keep the mucous layer intact. So does the presence of peace-keeping microbes such F. prausnitzii.
F.prausnitzii colonizes the mucous layer and produces by-products such as Butyrate [saturated fat is good-health promoting and down-regulates immune response]. Theses short-chain fatty acids seem to have an anti-inflammatory effect by reducing regulatory T cells which in turn control aggressive aspects of the immune system. The absence of F.prausnitzii and other microbes that perform similar functions often correlates with diseases such as IBS and obesity. Some of its relatives - clostridial clusters - have similar properties. [see image below]
Celiac and Gluten Sensitivity are associated with the following inflammatory problems:
- Thyroid disease
- Neurologic diseases
- Osteoporosis
- Decreased fertility
- Recurrent UTIs
- Autoimmune disease
- Skin disorders e.g. eczema, rosacea
- RLS – restless leg syndrome
The following changes in our modern food supply are linked to chronic complex disease:
- Sugar and refined grain flours, processed - high glycemic foods with high “carbohydrate density”
- Fructose from sugar and HFCS [a dose response]
- Increased processed-seed oils [Omega-6] relative to Omega-3 EFA intake
- Food sensitivities such as gluten, grains or dairy
- Insufficient vegetables [phytonutrients-epigenetics]
- Insufficient fiber [microbiome]
- Foods contaminated with environmental toxins such as game fish (mercury), non-organic fruits and vegetables with pesticide residues, BPA in plastics, Genetically Engineered foods
The Impact of diet in shaping gut microbiota revealed by a comparative study in children from Europe and rural Africa. African and European results were exactly opposite. Firmicutes are common in depression and obesity and are dominant in the European diet and far less present in the African diet.
The New Frontier will be found in the elegant inter-connections between the gut and all parts of the body. There are a growing number of examples connecting health problems to the microbiome, such as the emerging role of the gut in chronic heart failure. "Lack of mucosal integrity with consecutive local and systemic inflammation and dysfunction in transport proteins may worsen the clinical symptoms of chronic heart failure". [Curr Opin Clin Nutri Metab Care, 2008; 11:632-639]
REVERSE. It is possible to reverse and un-do the damage caused by disease in the gut by changing our behavior and following the Recommendations of The 5R Model to:
- Remove
- Replace
- Repair
- Reinoculate
- Rebalance
REMOVE.
- Elimination of disease causing microorganisms [dysbiosis] e.g. SIBO, yeast, parasites. Rx with appropriate agent e.g. Diflucan, Nystatin, Xifaxin. See FODMAPs example below
- Foods that one may be intolerant to [elimination diet: start with gluten and dairy]
- Medications that may negatively influence an optimal GI environment [such as PPIs, H2 blockers, NSAIDs, antibiotics, steroids]
- Stress: how we interpret and respond
Common FODMAPs include:
- Fructose: A simple sugar found in many fruits, vegetables and added sugars
- Lactose: A carbohydrate found in dairy products like milk
- Fructans: Found in many foods, including gluten grains like wheat, spelt, rye and barley
- Galactans: Found in large amounts in legumes
- Polyols: Sugar ALCOHOLS like xylitol, sorbitol, maltitol and mannitol. They are found in some fruits and vegetables, and often used as sweeteners.
REPLACE.
- Stomach acid using apple cider vinegar, Swedish bitters, Betaine HCL tablets 30-60 minutes before meals
- Digestive enzymes [plant-based], Pancreatic enzymes e.g. pancreas, Similase, GB digestion
- Choleretics [increase the secretion of bile from the liver], Ox Bile, dandelion root
REPAIR.
- Nutrient support with whole-foods, minimally processed, e.g. elimination diet or FODMAPS
- Zinc carnosine [protective]
- DGL-Deglycerinated Licorice, Slippery Elm
- Turmeric-Curcumin [will turn off your NfkB and that's a good thing]
- Glutamine [amino acid] 1,000 mg three times/daily
- Gelatin rich bone broths that are amino acid nutrient dense e.g. chicken, beef. Recommended reading: Nourishing Broth by Sally Fallon and Kayla Daniels PhD.
RE-INOCULATE.
- Administer probiotics from the following three families that have been found to be beneficial for GI function: Bifidobacteria, Lactobacilli, and Saccharomyces. Ther-biotic by Klaire
- Administer prebiotics (food that promotes beneficial bacterial growth) such as bananas, plantains, onions, asparagus and garlic, most vegetable-based fiber
- Fermented foods like sauerkraut, cabbage, kimchi, beets, yogurt, kefir
RE-BALANCE.
- Rest and relaxation-response
- Adequate sleep
- Meditation
- Yoga
- Tai chi
- Cognitive behavioral therapy
- Health coaching
For more "news to use" and the science to go with it, visit The Health Edge: Translating the Science of Self-Care. Not all research slides are shown in this article. To download complete lecture, follow this link to BHS Creating Health Wellness Series.
Balance.